(410) 764-7044
6506 Reisterstown Road, Baltimore
1205 York Road, Lutherville
6305 Belair Road, Baltimore
7809 Wise Avenue, Dundalk
July 2020
Preventing Plantar Warts
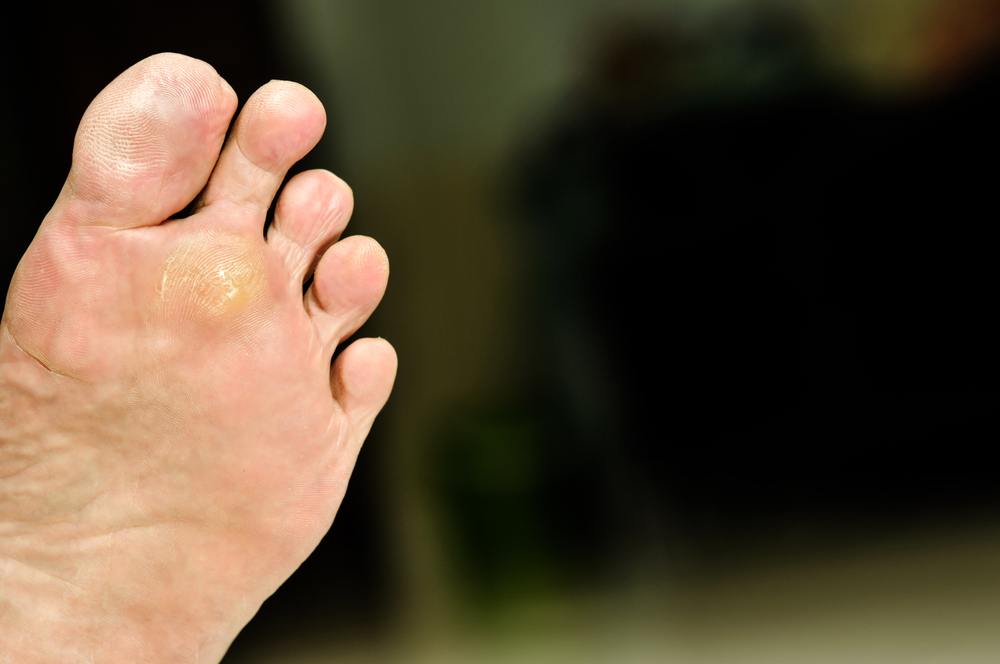 Warts on the bottom of the feet, known as plantar warts, are a common condition. About 25% of people get plantar warts at some point in their lifetime, often during childhood or adolescence. Plantar warts are caused by the human papillomavirus, also known as HPV, and can be highly contagious. To prevent plantar warts, avoid walking barefoot in damp public areas, such as community swimming pools or water parks. Wear clean cotton socks and change them regularly. Inspect your feet and take extra precautions if you notice a cut or scratch, as these may make you more susceptible to infection. If you or someone close to you has a plantar wart, it is suggested to keep it covered with a bandage in order to avoid spreading the virus to others. To avoid the risk of contagion or infection, it is recommended that you consult with a podiatrist right away.
Warts on the bottom of the feet, known as plantar warts, are a common condition. About 25% of people get plantar warts at some point in their lifetime, often during childhood or adolescence. Plantar warts are caused by the human papillomavirus, also known as HPV, and can be highly contagious. To prevent plantar warts, avoid walking barefoot in damp public areas, such as community swimming pools or water parks. Wear clean cotton socks and change them regularly. Inspect your feet and take extra precautions if you notice a cut or scratch, as these may make you more susceptible to infection. If you or someone close to you has a plantar wart, it is suggested to keep it covered with a bandage in order to avoid spreading the virus to others. To avoid the risk of contagion or infection, it is recommended that you consult with a podiatrist right away.
Plantar warts can be very uncomfortable. If you need your feet checked, contact one of our podiatrists from Plaza Podiatry. Our doctors will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our offices located in Baltimore, Lutherville, and Dundalk, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Wounds That Don't Heal Need to Be Checked
Exercise Can Benefit Patients With Peripheral Neuropathy
 Peripheral neuropathy, which can cause weakness, numbness, and pain in your feet, might make you reluctant to exercise. However, there is scientific evidence that you can benefit from physical activity. Researchers have found that exercising can improve balance, strength, and walking speed, reduce neuropathic pain and sensory disturbances, and improve mobility and confidence in patients with peripheral neuropathy. Doctors recommend that patients with peripheral neuropathy engage in flexibility, endurance, strength, and balance exercises to get maximum results. A podiatrist can help you maintain an active and healthy lifestyle by providing treatments to slow the progression of the disease, decrease your pain, and maintain the health of your feet.
Peripheral neuropathy, which can cause weakness, numbness, and pain in your feet, might make you reluctant to exercise. However, there is scientific evidence that you can benefit from physical activity. Researchers have found that exercising can improve balance, strength, and walking speed, reduce neuropathic pain and sensory disturbances, and improve mobility and confidence in patients with peripheral neuropathy. Doctors recommend that patients with peripheral neuropathy engage in flexibility, endurance, strength, and balance exercises to get maximum results. A podiatrist can help you maintain an active and healthy lifestyle by providing treatments to slow the progression of the disease, decrease your pain, and maintain the health of your feet.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with one of our podiatrists from Plaza Podiatry. Our doctors will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
- Numbness
- Sensation loss
- Prickling and tingling sensations
- Throbbing, freezing, burning pains
- Muscle weakness
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact our offices located in Baltimore, Lutherville, and Dundalk, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What Are Stress Fractures?
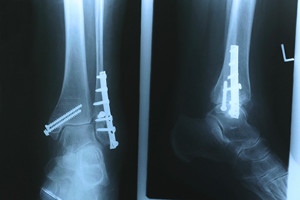 A stress fracture is a tiny crack in the bone that occurs because too much stress was placed on the foot. Stress fractures don’t usually occur because of a particular trauma, but rather they gradually develop over time. Some causes of stress fractures include repetitive high-impact activities, increased training, low bone density, and poor nutrition. Most stress fractures can be diagnosed with x-rays, but an MRI or CT scan may be necessary for smaller and newer stress fractures. Upon the discovery of a stress fracture, a cast or walking boot may be necessary. Generally, stress fractures take around 4-6 weeks to heal, and a slow return to your normal activity will be needed. If you are feeling a gradual increase of pain in the feet that you believe may be a stress fracture, please consult with a podiatrist for a proper diagnosis.
A stress fracture is a tiny crack in the bone that occurs because too much stress was placed on the foot. Stress fractures don’t usually occur because of a particular trauma, but rather they gradually develop over time. Some causes of stress fractures include repetitive high-impact activities, increased training, low bone density, and poor nutrition. Most stress fractures can be diagnosed with x-rays, but an MRI or CT scan may be necessary for smaller and newer stress fractures. Upon the discovery of a stress fracture, a cast or walking boot may be necessary. Generally, stress fractures take around 4-6 weeks to heal, and a slow return to your normal activity will be needed. If you are feeling a gradual increase of pain in the feet that you believe may be a stress fracture, please consult with a podiatrist for a proper diagnosis.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact one of our podiatrists from Plaza Podiatry. Our doctors can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our offices located in Baltimore, Lutherville, and Dundalk, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Older Adults and Heel Pain
 There are several bones, muscles, ligaments, and joints that each foot consists of. The feet absorb the weight of the body, and heel pain is experienced by many patients. The shape of the foot may change as the aging process occurs, so one may be vulnerable to developing specific foot conditions. These can include heel spurs, plantar fasciitis, and ankle injuries. It is beneficial to wear shoes that fit correctly in addition to having adequate cushioning in the heel area. There may be existing medical conditions that can lead to heel pain, consisting of certain types of arthritis, or obesity. Research as indicated it is beneficial to perform stretches that can help to loosen the muscles and tendons surrounding the heel, and this may help to relieve a portion of heel pain. If you have any type of heel pain, please consult with a podiatrist who can properly diagnose and treat this ailment.
There are several bones, muscles, ligaments, and joints that each foot consists of. The feet absorb the weight of the body, and heel pain is experienced by many patients. The shape of the foot may change as the aging process occurs, so one may be vulnerable to developing specific foot conditions. These can include heel spurs, plantar fasciitis, and ankle injuries. It is beneficial to wear shoes that fit correctly in addition to having adequate cushioning in the heel area. There may be existing medical conditions that can lead to heel pain, consisting of certain types of arthritis, or obesity. Research as indicated it is beneficial to perform stretches that can help to loosen the muscles and tendons surrounding the heel, and this may help to relieve a portion of heel pain. If you have any type of heel pain, please consult with a podiatrist who can properly diagnose and treat this ailment.
Many people suffer from bouts of heel pain. For more information, contact one of our podiatrists of Plaza Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our offices located in Baltimore, Lutherville, and Dundalk, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.







